Cancer Genetic Counselors Benefit Institutions Through Downstream Revenue
In 2012, hereditary breast and ovarian cancer syndrome (HBOC) and Lynch syndrome (LS) were recognized as Tier 1 conditions by the Center for Disease Control and Prevention1. These syndromes predispose to early onset cancers as well as multiple primary tumors. The identification of individuals with HBOC and LS is critical in implementing enhanced cancer screening and management with the goal of reducing cancer incidence and mortality. Genetic counselors (GCs) are trained professionals who play a vital role in identifying such patients. GCs coordinate genetic testing and counsel patients about their cancer risks as well as ways to mitigate these risks. In the United States, there are presently over 5,000 board-certified GCs, 59% of whom are involved in direct patient care. Of that sub-group, about 50% specialize in cancer2.
GCs are important marketing tools for their institutions; their service either brings a patient to the institution or contributes to increased revenue for an already established patient. While some private payers recognize GCs as billable providers, the Centers for Medicare and Medicaid currently do not3. Therefore, the financial impact of GCs within a healthcare institution have to be evaluated using other means.
Study and Methods
To determine the downstream revenue that is generated by a cancer genetic counselor, Mauer et al recently conducted a retrospective chart review identifying patients with HBOC and LS seen in the UT Southwestern Medical Center Cancer Genetics Clinic between November 1, 2009 and January 31, 20194. Genetic counseling sessions were not billed during the duration of the study and therefore, revenue from these consultations was not included. In addition, external laboratories performed the genetic testing for which GCs did not receive remuneration. Total revenue was calculated for each patient before and after they met with a GC. Patients who did not receive any clinical services at the institution after the time of their genetic counseling visit were excluded from the study. The revenue per patient per GC was calculated using available national statistics.
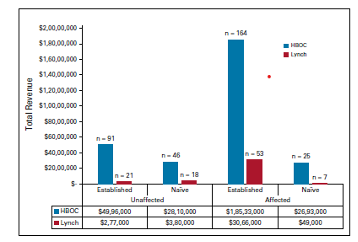
Results
Overall, the downstream revenue generated from the 425 patients in this study with HBOC or LS mutations totaled $32.8 million after their cancer genetics appointments. Patients unaffected with cancer (n=176) generated $8.4 million, while patients whose first visit to the institution was for a genetic counseling consultation (n=96) generated $5.9 million. The total revenue generated for the entire study population, broken down by syndrome, patient type and cancer status is reflected in the figure on the right.
This is the first study to determine the downstream revenue for an institution following the identification of cancer susceptibility pathogenic mutation carriers by a GC. Furthermore, it is anticipated that the revenue brought in by a GC is even more than the data presented in this study given the advent of next-generation sequencing panels and the identification of many pathogenic mutations in other genes. The revenue generated by patients who had never visited the institution prior to their genetic counseling appointment was notable. These are patients who might have never received care at the institution if not for their genetic counseling visit, which highlights a very important benefit that cancer GCs provide.
In conclusion, this study suggests that “the value of GCs cannot be limited to revenue generated only through consultation fees or test utilization management. Furthermore, through evidence-based preventative services recommended by a GC, insurance companies can reduce their payments for healthcare costs incurred by expensive
cancer treatments. Finally, and most importantly, the recommendations of a cancer GC help contribute to a reduction in cancer incidence and mortality, ultimately helping to save lives.”
Should you have any questions or would like further information, please contact Nancie Petrucelli at (313) 576-8704/[email protected].
back to blog